Erstmaßnahmen
Reversible Ursachen (DD: Trauma-CPR)
CPR-Quali optimieren!
Textbaustein Übergabe Reanimation/ROSC
Übergabe von RTW+NEF im Schockraum unter laufender Reanimation (OHCA) via Corpuls CPR® / LUCAS® // nach primär erfolgreicher präklinischer Reanimation (OHCA). Situation: ### - Kreislaufstillstand beobachtet: JA / NEIN - Laienreanimation: JA / NEIN / INSUFFIZIENT - Eintreffen RD ### min nach Alarm - No Flow Zeit geschätzt: ### Initialer Rhythmus: VF / ASY / pVT / PEA - Anzahl Defibrillationen: ### - Amiodaron/Lidocain kumulativ: ### mg - Adrenalin kumulativ: ### mg - Weitere Medikamente präklinisch: ### - Zugänge präklinisch: i.o. Tibia RECHTS/LINKS / 20G ### - Atemwessicherung: LT / LaMa / ETI - Magensonde: Nein / Ja, via SGA/oral/nasal Gesamtdauer Reanimation bis Übergabe: ### min - etCO2 bei Übergabe: ### mmHg - Rhythmus bei Übergabe: ### - Soziales: ###
Textbaustein Untersuchung+POCUS Reanimation/ROSC
Pat. männlich/weiblich ca. ____ Jahre, Z.n. Reanimation mit aktuell ROSC / unter laufender Reanimation. - A: Frei, Verlegt durch Blut/Erbrochenes, präklinisch gesichert / Sicherung im Schockraum mit Larynxtubus / Larynxmaske / ETT Gr. ____, fixiert bei ____ cm Zahnreihe / Mundwinkel. Cuffdruck: _____ cmH2O, etCO2 pos. - B: Atemgeräusch seitengleich, etCO2 ______ mmHg, beatmet mit FiO2 1,0 / 0,5 / 0,3 DuoPAP / CMV / ASV, Thorax instabil mit Krepitationen nach Herzdruckmassage, sonografisch 2./3. ICR MCL seitengleich Pleuragleiten darstellbar - C: Pulse radial / femoral / A. Carotis schwach / kräftig tastbar, RR nicht messbar / RR messbar mit ____ mmHg unter ______ µg/kg/min Adrenalin/Noradrenalin, Recap ____ s zentral. Sonografisch von subxiphoidal keine Perikardtamponade, V. Cava kollaptisch / gefüllt / prall, Kammerflimmern / insuffiziente mechanische Aktion/ keine mechanische Aktion / Ventrikelthrombus / orientierend ausreichende EF. Lactat erste BGA ____ mg/dl, Hb ___ g/dl. - D: Pupillen isokor, weit, LR prompt / träge / lichtstarr, BZ in BGA ____ - E: Temp. ____ °C, keine weiteren Verletzungen erkennbar, keine Beinödeme, keine Beinumfangsdifferenz, Kalium BGA ____ mmol/l, pH BGA ____
Textbaustein ECPR
Bei beobachtetem Kreislaufstillstand mit suffizienter Laienreanimation, mutmaßlich thromboembolischer Genese, Alter <75 Jahre und Fehlen von Kontraindikationen bestand die Indikation zur extrakorporalen Kreislaufunterstützung. Sofortige Verlegung ins Herzkatheterlabor unter laufender mCPR via Corpuls CPR® zur Anlage VA-ECMO.
Textbaustein Abbruch Reanimation
Trotz leitliniengerechter Reanimation über ### min konnte kein suffizienter Spontankreislauf etabliert werden. Ausschluss reversibler Ursachen des Kreislaufstillstands. Im interdisziplinären Konsens infauste Prognose. Beendigung der Reanimationsmaßnahmen und Todesfeststellung um #### Uhr. ###ODER Abbruch nach 1. BGA Bei pH ###, unbeobachtetem Kreislaufstillstand, unklarer Liegedauer, fehlender/insuffizienter Laienreanimation, Asystolie, etCO2 unter optimaler CPR <10 mmHg, sonografisch vollständigem mechanischem Herzstillstand mit Ventrikelthrombus, niemals ROSC, ###WEITERES. Im interdisziplinären Konsens infauste Prognose. Beendigung der Reanimationsmaßnahmen und Todesfeststellung um #### Uhr. ###ODER Fortführung der Reanimation war gemäß der im Verlauf vorliegenden Patientenverfügung / gemäß der durch die vorsorgebevollmächtigten Angehörigen glaubhaft und nachvollziehbar vorgebrachten Einschätzung nicht vom Patientenwillen gedeckt. Beendigung der Reanimationsmaßnahmen und Todesfeststellung um #### Uhr. ###UND Die Angehörigen ###WER? wurden von uns persönlich/telefonisch über den Todesfall informiert. ###NATÜRLICH: Bei ### nachvollziehbare Kausalkette und somit a.e. natürliche Todesart. Die Angehörigen stimmen einer Sektion zu / lehnen eine Sektion ab. ###SONST: Bei nicht natürlicher / ungeklärter Todesart informierten wir die Kriminalpolizei (### Uhr), die den Leichnam beschlagnahmte.
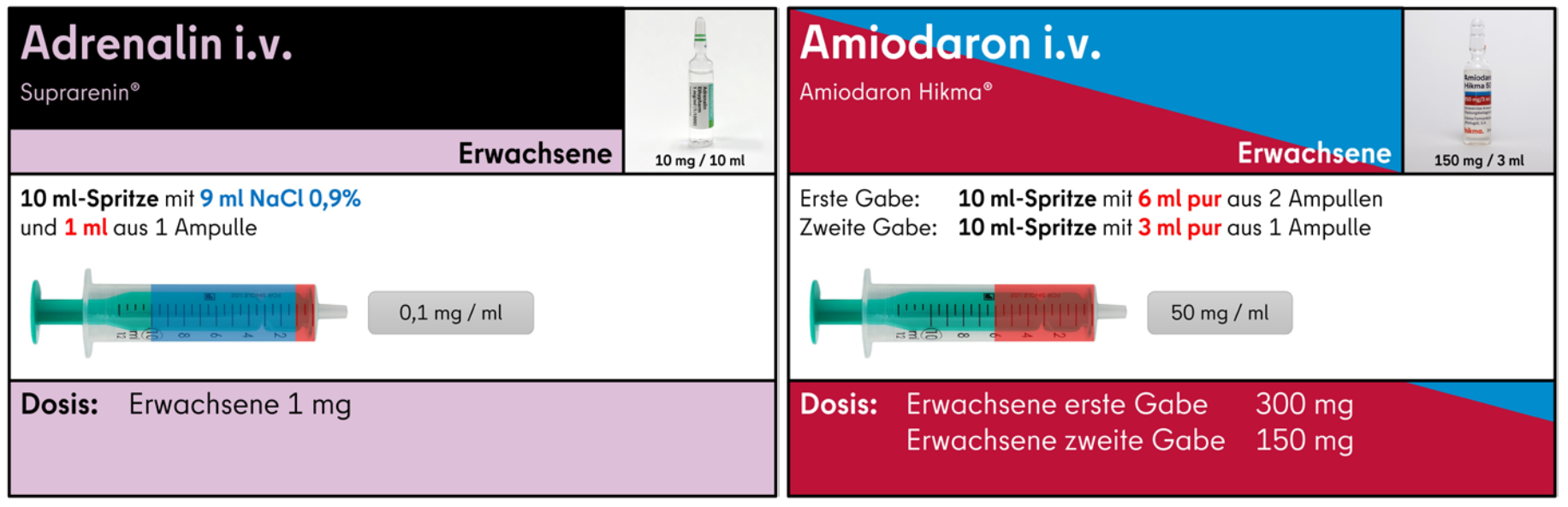
Aufziehhilfen
Literatur
- Carotid Continuous Doppler1
- CPRIC
- Primär Asystolie 0.6% gutes neurolog. Outcome2 – Vergleich Thorakotomie 👀
- Ohne LVOT-Öffnung im TEE kein ROSC3
- Intra-Arrest Transport erhöht Mortalität4
- Kleine BVM Bags helfen nicht5
- Ventilation matters!6
- Herzkatheter-Management AHA Statement7
- CPR inkl. Defib geht in Bauchlage8
- TV Medical Dramas machen Laien schlechter in CPR9
- TOR
- HDM auf fahrender Trage ist genauso effektiv wie normale HDM10
- Arrest in ZNA: Gutes Outcome bei unvorhergesehenen im Vergleich zu bereits vorher instabilen11
3-Phase-Model of Cardiac Arrest12
- Electrical Phase 0-4 min: Defibrillation
- Circulatory Phase 4-10 min: Braucht Rezirkulation (HDM), diastolische Drücke bevor ROSC
- Metabolic Phase >10 min: TTM effektiv?
Footnotes
-
Zhao. Resuscitation 2024. A new method to evaluate carotid blood flow by continuous Doppler monitoring during cardiopulmonary resuscitation in a porcine model of cardiac arrest. ↩
-
Dwivedi. Resuscitation 2025. Incidence and outcomes of out-of-hospital cardiac arrest from initial asystole: a systematic review and meta-analysis. ↩
-
Association between left ventricular outflow tract opening and successful resuscitation after cardiac arrest. Catena, Emanuele et al. Resuscitation, Volume 138, 8 - 14 ↩
-
Grunau B, Kime N, Leroux B, et al. Association of Intra-arrest Transport vs Continued On-Scene Resuscitation With Survival to Hospital Discharge Among Patients With Out-of-Hospital Cardiac Arrest. JAMA. ↩
-
Snyder. Resusciation 2023. Association of small adult ventilation bags with return of spontaneous circulation in out of hospital cardiac arrest ↩
-
Chang. Resuscitation 2019. Association of ventilation with outcomes from out-of-hospital cardiac arrest ↩
-
AHA. 2023. Cardiac Catheterization Laboratory Management of the Comatose Adult Patient With an Out-of-Hospital Cardiac Arrest: A Scientific Statement From the American Heart Association ↩
-
Anez. Anesthesia & Analgesia 2021. Cardiopulmonary Resuscitation in the Prone Position in the Operating Room or in the Intensive Care Unit: A Systematic Review ↩
-
Colwill. Postgrad Med J 2018. Cardiopulmonary resuscitation on television: are we miseducating the public? ↩
-
Hung-chih Chen, Yi-chieh Chen, Po-jung Chen, Ying-jia Lin, Yi-chen Chen, Chung-han Ho, Chen-wei Wu, Chien-chin Hsu, Yi Lin, Yu-hui Lin, Hsin-min Lee, Chang-chih Tsai. Characteristics, etiologies and outcomes of cardiac arrest in the emergency department. Signa Vitae. 2026.doi:10.22514/sv.2026.001. ↩
-
JAMA 2002;288(23):3035 ↩